Dr. Paul Wilson Featured on Elevator Podiatrist Podcast Episode 4
August 5, 2019
Becoming a Podiatrist and What to Expect During Your First Visit - Dr. Paul Wilson

Q&A Transcript
Joe Crosby:
00:14 Welcome to the elevator podiatrist, the show where we ask common foot and ankle questions to top podiatrists from around the country. There's no appointment or copay required for this one on one Q&A, only free advice from individuals who have devoted their lives to all things feet, I'm your host Joe Crosby. And today I'm joined by Dr. Paul Wilson podiatrist out of Union City and Dyersburg, Tennessee. What's your favorite foot deformity or condition that you, that you get to treat kind of on a daily basis or you know, maybe a rare one that you'll see, you know, once every few years.
Dr. Paul Wilson:
00:52 What I like most about being a podiatrist is the fact that I can get patients better almost all the time. Usually with very simple interventions. As far as my favorite area of the foot, I really liked the first metatarsal phalangeal joint or the big toe joint. So I think the pathologies are very interesting to study and very interesting to treat. And it's one of the main areas that we do see pathology, in the foot.
Joe Crosby:
01:27 And we had discussed talking about the educational process, you know, what it takes to become a podiatrist. So what, what is that process? What's, what is the educational process of becoming a podiatrist?
Dr. Paul Wilson:
01:39 Well, it's quite extensive as you might imagine, though I have had patients ask me if I went to college, but it's true, the vast majority of podiatrists have a four year degree, usually in the natural sciences such as biology or chemistry and all those as are not that necessarily true. I had a classmate that was a French major actually. So, upon completing the four year degree, candidates are admitted to podiatric medical school, which is four years in duration and is modeled exactly like allopathic or osteopathic medical schools. In fact, uh, the, uh, the podiatry school that I attended is also an osteopathic medical school. And my classmates were also studying to be osteopathic physicians.
Joe Crosby:
02:41 What is osteopathic?
Dr. Paul Wilson: 02:43 A osteopathic is a medical degree that is the DO degree. So physicians that have MD degrees and traditions that have DO degrees and the physicians with the DO degrees are the osteopathic physician. So they have just a little bit different philosophy than the allopathic chow counterparts. Uh, usually I have a more holistic approach rather than a focused approach to a particular body system. Upon completing four years of podiatry school, the graduate enters into residency training, which is now a uniformly three years in length. So there's been a lot of work over the last 20 or so years to standardize the advanced residency training so that they're all very similar and all podiatrists should be regarded as surgical subspecialists that have been to residency training. So in all that is at least 11 years of total education.
Joe Crosby:
03:52 So every podiatrist would be considered a surgeon? Is that what you would say?
Dr. Paul Wilson:
04:00 Any podiatrist that has completed residency training in the past 20 or 25 years should be regarded as a surgical subspecialists. Yes.
Joe Crosby:
04:09 Okay. So with that advanced surgical training, I'm sure there are different subsets of surgery that you can perform. So what additional treatments and services does that allow you to perform? And what would be some of those subsets of surgical specialties?
Dr. Paul Wilson:
04:28 Well, even though that training is standardized across the nation, the actual scope of practice that's imposed by the state is highly variable. So some podiatrists are restricted to only the foot or certain areas of the foot. While other states allow podiatrists to perform surgery on the ankle or even soft tissue procedures into the leg. So not only is there a variability amongst states, there can also be some variability from community to community based on what hospital privileges are granted in that locality. So that's where the variability comes in, so though the residency is pretty much standardized at this point. I have found that podiatrits tend to gravitate towards an area of clinical interest and so forth, rather than a formal specialty within podiatry. For example, many podiatrists prefer to do wound care. Many podiatrists prefer to do biomechanics, some podiatrists prefer to focus on sports medicine. While there's some fellowship training available in those areas, it's not common for doctors to pursue fellowship training and they just more or less pursue their areas of clinical interest.
Joe Crosby:
05:55 And what's kind of your area of interest would you say?
Dr. Paul Wilson:
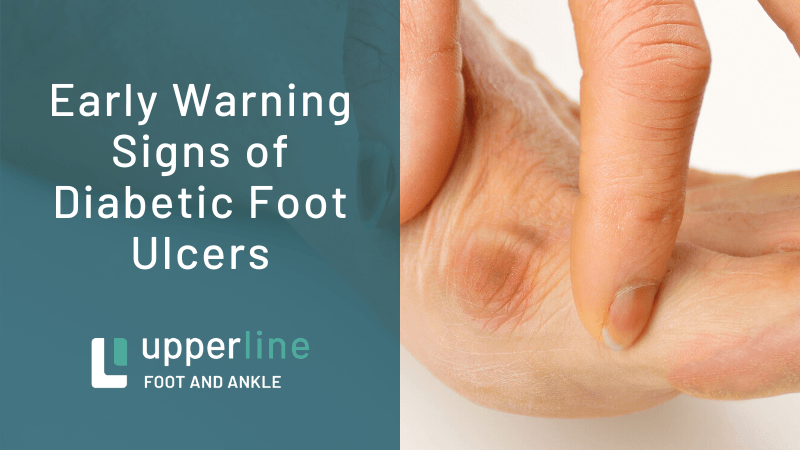
05:59 I'm very interested in neurological diseases that impact the foot. I'm interested in how altered biomechanics result in foot ulcers, which is very interesting to me. And again, I'm interested in diseases of the big toe joints such as, buneons, which is also known as hallus valgus, or severe arthritis of that area.
Joe Crosby:
06:25 So during your training and in schooling, I'm sure there were some hands on training involved probably near the end. What, what type of hands on training did you get while in school? And how early did you start preferring performing surgical procedures on actual patients?
Dr. Paul Wilson:
06:42 The clinical phase of podiatry education begins in the third year for podiatry School just like the allopathic and osteopathic counterparts. So a lot of that is attending clinics, attending patients in the hospital and then as far as residency training goes, the rotations are pretty diverse. So I had very solid rotations in general surgery, vascular surgery and the inpatient hospital medicine as well as wound care.
Joe Crosby:
07:12 Next would be the continued training. So now you're a practicing podiatrist, what other training do you kind of do on an ongoing basis to kind of stay up to date to, you know, learn new things? You know, stay on top of new trends?
Dr. Paul Wilson:
07:26 Well, it's practically impossible to do it on your own. You have to rely on your colleagues to help with that. So it's actually usually in the form of seminars and conferences that occur across the country and usually have time to go one or to go to two per year, which more than meets the mandated continued educational requirements. But, uh, I found that it's, it's best to, uh, take, take a few days away and focus on updating and refreshing.
Joe Crosby:
08:02 Moving more towards the day to day working with patients, you see a lot of different foot issues from wounds to ingrown toenails to buneons. There's a lot of home remedies out there that, you know, on the Internet that probably worked pretty well for most people. But in what instances would you suggest someone actually come in to see a foot specialist?
Dr. Paul Wilson:
08:21 Well, that's highly variable, I would say Joe, but usually when something gets to the point that you can't ignore it any longer so that there are many signs. Usually people know right away that something is wrong. There's pretty good indicators of things that have gone wrong in the human body. And one of the earliest warning signs that we have is pain. So pain that continues and is unresolved usually needs to be addressed or evaluated.
Joe Crosby:
08:57 So a lot of people have never been to a podiatrist before and they may know, they may know what it is, they may know what a podiatrist does. They know a podiatrist does ingrown toenails or you know, deals with foot wounds. But when a new patient is coming in, what should they expect during their first appointment?
Dr. Paul Wilson:
09:16 Well, I think it be very similar to other doctor's appointments. So normally when you arrive into the office, especially if you're new patients, there's a check in procedure and the dreaded new patient paperwork that is pretty comprehensive. Once the patient is taken back to the room, you are usually first seen by one of our medical assistants that reviews the complaint. And eventually when you see the doctor, the doctor will ask you many questions, not only about what's going on with your foot, but also what's going on within your health in general. Because foot complaints can also be a sign of a disease process elsewhere in the body. It is important to pick up on that right away. So after the doctor takes a history, the doctor will conduct the physical exam, not only of the foot, but also of some other systems including a skin assessment, a vascular assessment and the neurological assessment. There may or may not be x-rays or there may or may not be other diagnostic testing in the office. So once the doctor has taken a history and physical, it's the doctor's responsibility to arrive at the diagnosis and formulate the treatment plan.
Joe Crosby:
10:43 Earlier you mentioned one of your kind of areas of interests was neurological issues as related to the feet. What would be an example of a neurological issue that would relate to the feet and during your assessment, what would you kind of look for?
Dr. Paul Wilson:
10:59 This may be a little bit too technical, but again, I try to evaluate the patient's symptoms, any particular pattern of symptoms, any particular distribution of symptoms. And I try to correlate that with my physical exam. So I do a pretty complete neurological exam on patients that come in with the neurological type complaints, things like muscle weakness, numbness, tingling, Paresthesias, difficulty walking, things like that.
Joe Crosby:
11:36 We all know how important is to brush and floss our teeth every day. That's literally been hammered into our brains since we were kids. But daily foot care hasn't really been ingrained into our daily habits, even though something like three quarters of Americans will experience foot pain or some kind of put issue during our lives. So what are some general day to day foot care tips that you'd like to see everyone follow? You know, comparable to like brushing our teeth?
Dr. Paul Wilson:
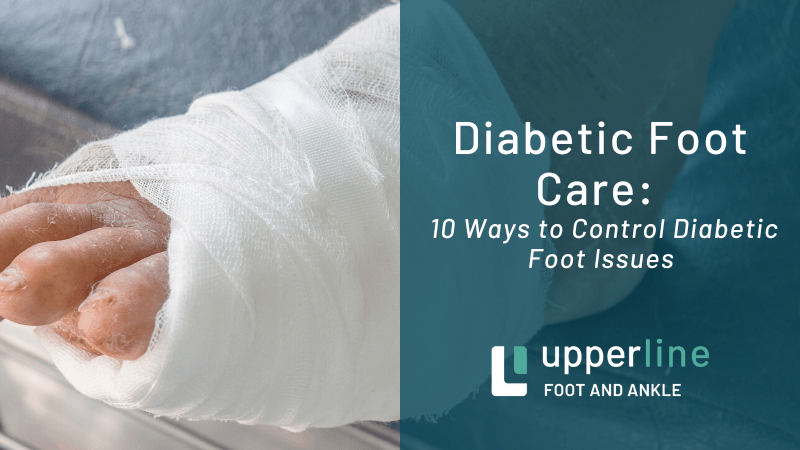
12:01 Okay. Well I think that's a great question. I see a lot of Fungal infections in between the toes and so forth. And this is mainly in my opinion due to accumulated moisture or a failure to get the foot completely dry after showers and baths. So if most people, I think when they get out of the shower or the bathtub, they start at their head and start working their way down. And by the time they get down to their feet, they're either just decided they're moving on with their day or they're drying their feet off with something that's already pretty damp. And then the next thing that go on is the shoes and socks, which entrap that moisture. So I would say probably the best thing people, the average person can do for their feet is make sure they're getting their feet completely dry after their bathing routine.
Joe Crosby:
12:55 I want to thank Dr. Wilson for speaking with me today, and I want to thank you for listening to the elevator podiatrist.